2026-02-10 • 11 min
Trigger points: referred pain, causes… and how to release them
A clear guide to trigger points: why they appear, how they cause referred pain, what helps (self-release, mobility, massage) and when to seek help.
When a “knot” sends pain elsewhere: neck, jaw, back, glutes…
Trigger points explained (and how to avoid overdoing it)
A trigger point is often described as a painful “knot” in a muscle — but its hallmark is referred pain (pain felt somewhere else). The goal isn’t to “break” anything: we aim to reduce protective tone, calm the nervous system, and restore easy movement.
Simple, useful definition
A trigger point is a hypersensitive spot within a muscle (often in a tight band) that can produce local pain, referred pain, and restricted movement.
- Common in neck, traps, shoulder blade area, low back, glutes and calves.
- Often linked to stress, fatigue, posture or overload.
- Pain may be felt away from the pressed area (classic signature).
- Precision + gentleness + consistency often work better than force.
Why they appear (most common causes)
Stress + upper-chest breathing
When the nervous system stays in alert mode, some muscles hold background tension (shoulders, neck, jaw).
Posture and repetitive patterns
Desk work, driving, phone use, repetitive sport: the muscle is loaded in the same range and gets sensitized.
Fatigue / poor recovery
Sleep, hydration and overall load matter. A tired muscle becomes more reactive and tender.
Old pain / compensation
After pain or injury you move differently. Compensation patterns can create trigger points elsewhere.
How to recognize a trigger point (typical signs)
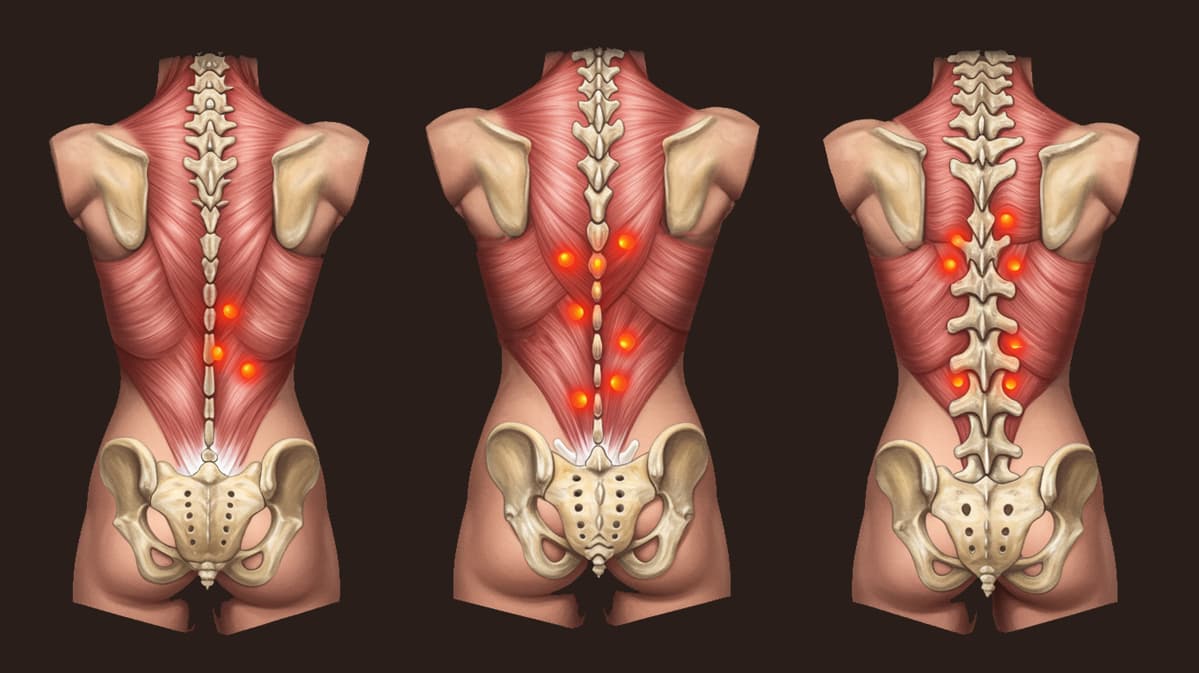
Pain reproduced by pressure
Pressing a specific spot recreates your “signature” pain (often very recognizable).
Referred pain
Pressure triggers pain that travels to another area: temple, arm, upper back, leg…
Stiffness + limited movement
You can move, but it feels braked, especially after sleep or long sitting.
Local fatigue / heaviness
The area feels overloaded or quickly fatigued even with normal activity.
Referred pain: common examples
These examples don’t replace diagnosis, but they explain why pain can be felt away from the real source.
Area
Traps / neck
Felt pain
Temple, head, behind the eye
Note
Common with stress + screens, often linked to shallow breathing.
Area
Chest / pecs
Felt pain
Front of shoulder / arm
Note
Can mimic shoulder pain; often with rounded posture.
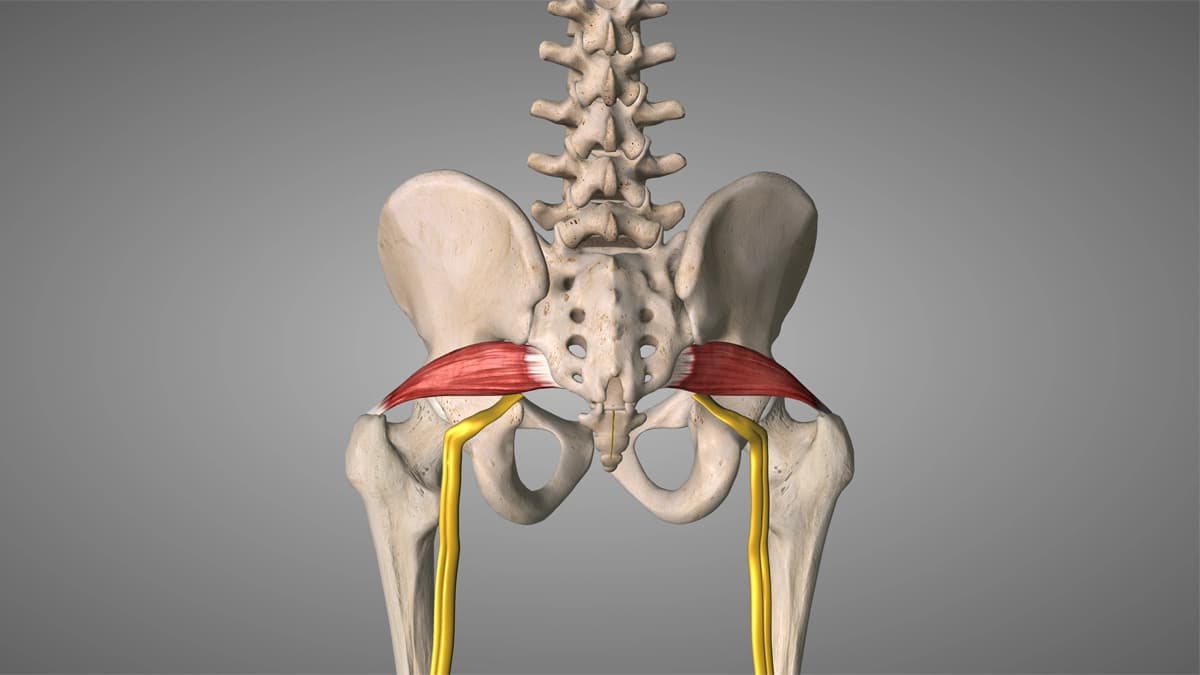
Area
Glutes (piriformis / glute med)
Felt pain
“Pseudo-sciatica”: buttock → back of thigh
Note
Sometimes confused with true sciatica; check neurological signs.
Area
Calves / foot
Felt pain
Heel / arch
Note
Common in walkers/runners or prolonged standing.
Self-release: a safe method (more effective than pain)
Goal: reduce sensitivity and restore movement. 60–90 seconds per point, 1–3 points per area, then gentle movement.
1) Find the precise spot
Look for a small, specific area — not a big surface. The pain should be recognizable.
2) Moderate pressure + breathing
Apply strong-but-breathable pressure (ball/knuckles/thumbs). Long exhale, relax jaw, let the body soften.
3) Micro-movements
Keep the pressure and add small slow movements (shoulder/hip/neck) to restore glide.
4) Reintegrate with movement
Afterwards, do 1–2 minutes of gentle mobility or walking. This often “locks in” the improvement.
- Max pain: 6–7/10. If breathing locks, it’s too much.
- No bruising: excessive pain increases guarding and can worsen it.
- Hydration + sleep matter more than any tool.
- If symptoms radiate with numbness/tingling: stop and get checked.
Massage: why it helps (when done well)
Massage can be very effective for trigger points when intensity is controlled and the nervous system is addressed (pace, breath, downshifting).
- Precise + slow work reduces defensive response.
- Chain approach treats drivers (posture/stress), not only symptoms.
- More stable results when you move a bit between sessions.
Common mistakes (that slow progress)
Going too hard
A trigger point isn’t a nail. Too much force makes the body guard and the pain returns faster.
Treating one spot and ignoring the cause
If stress, posture or training load don’t change, it keeps coming back.
Forgetting breathing
Often the #1 lever: long exhales reduce protective tone.
Confusing muscle pain with nerve signs
Radiation + numbness/weakness = don’t gamble, check it.
When to seek help
- Persistent numbness, weakness, electric sensations
- Sudden sharp pain or pain waking you at night
- Pain that progresses despite rest and smart adjustments
- Recent trauma (fall/accident) or fever/infection
Trigger points FAQ
Is a trigger point just a knot?
“Knot” is a simplification. Key idea: a hypersensitive spot that can create local pain and referred pain. Precision and gentleness usually beat force.
Why does it hurt somewhere else?
That’s referred pain: certain muscles have projection patterns. Find the source, not only the painful area.
Tennis ball or foam roller?
Both work. A ball is often more precise. In all cases: moderate, slow, breathable pressure.
How long until improvement?
Sometimes immediately. For stability (posture/stress), expect 2–4 weeks of consistency.
Want to treat neck/back/glute tension properly?
Send: your area (city) + your symptoms/tension + 2 time slots. I’ll reply quickly.
Book your massage
Send your area + your goal + 2 time slots, I’ll reply quickly.
Contact me →